LEARN HOW HIV IS COMMONLY TRANSMITTED
HIV can only be transmitted from someone living with HIV to another person through direct contact of the following bodily fluids:
- Blood (including menstrual blood)
- Semen / cum / precum / ejaculate
- Vaginal secretions
- Breast milk
Blood contains the highest concentration of the virus, followed by semen, followed by vaginal fluids, followed by breast milk. If a person living with HIV is taking HIV medications and has a durably suppressed viral load <200 copies/mL, they will not transmit HIV to others.
Taking an HIV test is the only way to know your HIV status. Make it a habit to get tested every three to six months if you’re sexually active or if you inject drugs.
Activities that transmit HIV
HIV may pass from one person to another any time there is contact with semen, pre-cum, vaginal fluids or blood. HIV is transmitted during sex and when using injection drugs and sharing needles. Mothers can also transmit HIV to their babies before or during birth or while breastfeeding, although this is very rare in the U.S. and in other places where mothers living with HIV have access to health care services.
People living with HIV who are taking HIV medications and have a suppressed viral load (who are “undetectable”) do not transmit HIV. People who are HIV-negative can prevent HIV infection with PrEP.
Bodily fluids that are NOT infectious:
- Saliva / spit
- Tears
- Sweat
- Feces / poop
- Urine / pee
Remember: Any body fluids that also contain blood may be infectious.
Sexual Intercourse
HIV may be transmitted during condomless sex if one partner living with HIV has a detectable viral load and the person who is HIV-negative is not taking PrEP. In the penis, vagina and anus, HIV may enter through very small cuts or sores or directly through the mucous membranes.
ORAL SEX
Oral sex is considered a low-risk practice. The virus can’t survive well in the mouth (in semen, vaginal fluid or blood), so the risk of HIV transmission through the throat, gums and oral membranes is low. Having an STI, cuts or mouth sores, recent dental work or bleeding gums may increase the likelihood that HIV may be transmitted during oral sex if the partner living with HIV has a detectable viral load and the person who is HIV-negative is not taking PrEP.
SHARING INJECTION NEEDLES OR WORKS
Sharing needles is considered high risk in terms of HIV transmission. If a person living with HIV injects with a needle then shares it with another person, the second person may become infected with HIV.
MOTHER-TO-CHILD
Mother-to-child transmission is now rare in the U.S. and other high-income countries because pregnant women are routinely tested for HIV infection, and those women who are living with HIV are given medications to prevent the fetus from getting infected, in particular during the latter months of pregnancy and during childbirth itself. Without such antiviral therapy, it is possible for an HIV-infected mother to transmit HIV before or during childbirth or later, through breast milk.
Take Care of Your Health: Know Your Status
Think you may be at risk for HIV infection? We can help. Learning your HIV status is the first step toward taking care of your health, no matter what the test result. Remember, very effective treatments are available to help you stay healthy if you test positive for HIV.
FIND A TEST
- We offer free, confidential HIV & STI testing at a number of locations in San Francisco.
- Use the Locator Tool on HIV.gov to find a testing site near you.
- You can also ask your doctor or medical provider for an HIV test.
TYPES OF HIV TESTS
- If you are sure or nearly sure you were exposed to HIV very recently, consider asking for an RNA test. HIV RNA tests can detect fragments of the virus within 10 to 14 days after exposure to HIV. Ask if you should consider post-exposure prophylaxis (PEP). Try to share as much as possible about what you were doing when you were potentially exposed to HIV so that your HIV test counselor can help you evaluate your risk.
- If you aren’t sure, a standard HIV antibody test gives accurate results within four to six weeks. It can take up to three months for your body to produce enough antibodies to HIV for the test to be accurate, so, using the HIV antibody test, you can’t be sure you’re negative until three months after exposure.
For more information about “window periods,” visit our HIV FAQs.
Get Tested Every Three Months
What’s the best time to get tested for HIV and STIs? We recommend people who are sexually active and people who inject drugs get tested for HIV and sexually-transmitted infections (STIs) every three to six months.
Establishing a regular testing schedule for yourself is a great way to take charge of your sexual health. Encouraging your regular sex partners to do the same is a great way of helping your partners and the community.
If you live in San Francisco or the Bay Area, stop by any of our locations for free HIV and STI testing. A counselor will be able to recommend a testing schedule for you. Schedule tests far in advance so they become routine.
Get Tested
IF YOUR TEST COMES BACK NEGATIVE
- Schedule a follow-up test. If you had an HIV antibody test less than three months after you might have been exposed, you should plan to get tested again to make sure you’re negative. See our FAQs about testing windows.
- Re-think your risk. Think about what puts you at risk for HIV and consider strategies to reduce your risk. We offer a program for people who are thinking about changing their substance use, for example.
- Test and repeat. Make regular HIV and STI testing part of your healthy sex life. We recommend that people get tested every three to six months. If you had an appointment at one of our sites, you can book your next appointment now.
- Consider PrEP. If sex puts you at high risk for HIV, a prevention strategy called PrEP (pre-exposure prophylaxis) might be a good fit. PrEP involves taking a medication to prevent HIV. Learn more about PrEP and ask your doctor if it’s right for you. (Be aware that PrEP only works against HIV, not other STIs like syphilis and gonorrhea.)
IF YOUR TEST COMES BACK POSITIVE
- Don’t panic. Remember, HIV today is a manageable disease. With good and consistent care, you can live a long and healthy life.
- See a doctor, even if you don’t feel sick. HIV does not always trigger symptoms, even for years, but the sooner you begin treatment the better your health will be.
- Find a support system. The emotional and physical challenges ahead can be difficult, and having people around to help is important. We offer a variety of services for people living with HIV, including support groups, information sessions and weekend retreats.
- Become undetectable to prevent HIV transmission. People who take their HIV medications every day suppress their viral loads to undetectable levels. People who are undetectable do not transmit HIV to partners. Read more about undetectable.
More HIV Resources
More Sexual Health Services

Which PrEP medication is best for me?
There are four different FDA-approved medications for PrEP: Truvada, Descovy, Apretude, and...

About Yeztugo – Downloadable Flyers
Yeztugo (lenacapavir) is a long-acting injectable version of PrEP Injections are given every...

Gender-inclusive sexual health brochures
PrEP Facts: Introduction & FAQ
Learn more about Pre-Exposure Prophylaxis (PrEP) and how this HIV prevention strategy may be useful for you or someone you know.
Landscape of Options for Oral PrEP
A generic version of a medication used for oral PrEP is now available. Here’s what to know — and what to do if you run into any payment issues at the pharmacy.
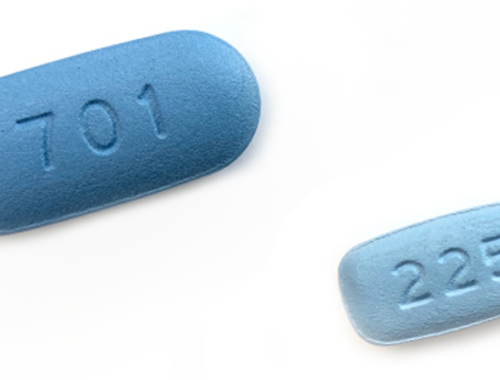
Info sheet: Which PrEP medication is best for me?
Two different medications are now FDA-approved for PrEP in the US: Truvada and...

Side-by-side comparison: Truvada and Descovy for PrEP
There are now two medications approved by the US Food and Drug Administration (FDA) for PrEP:...
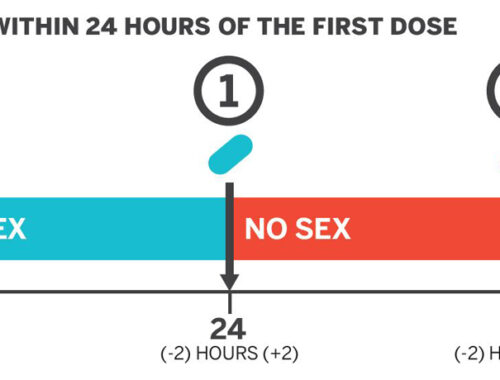
Info sheet: PrEP 2-1-1
Find out more info about how to take Truvada for PrEP 2-1-1 with this downloadable info...





