In SF, HIV care has suffered during COVID-19

In August 2021, the San Francisco Department of Public Health released the 2020 HIV Epidemiology Annual Report. While in recent years the report has been a cause for celebration as new HIV infections continued to decline, this year’s report paints a still incomplete picture of disruptions in HIV care caused by the COVID-19 pandemic. And, the report highlights the need for a renewed focus on ramping up HIV testing, prevention, and care in the coming year.
“The big picture is that HIV prevention and care has suffered during COVID-19,” said Janessa Broussard, NP, MSN, AGNP-C. “Early on in the pandemic, a lot of the smaller HIV clinics and testing programs closed due to the major challenges to provide care safely when little was known about SARS-CoV-2. A lot of people lost access or didn’t access services during shelter-in-place. SFAF received a lot of calls from individuals who did not have a place to go for HIV care. It’s going to take some time to really see the impact of COVID-19 on people living with HIV and the care they’ve received, but we know community testing and treatment programs need more support. This work is more important than ever.”
Decline in new HIV infections
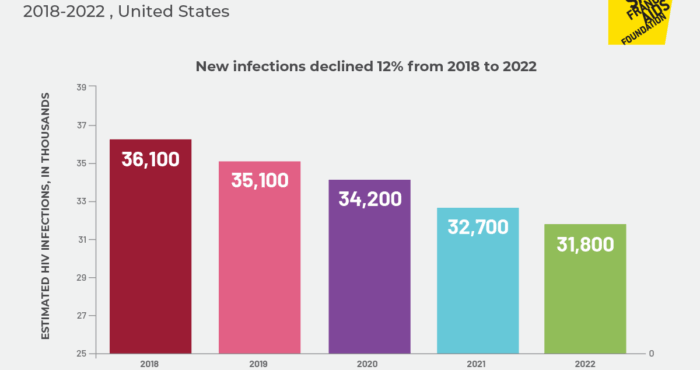
Since the scale-up of PrEP, San Francisco has celebrated a declining number of new HIV infections every year, with declines averaging around 16% since 2012. Last year continued this same downward trajectory, with a 22% decline in new HIV diagnoses from 2019 (168 diagnoses) to 2020 (131 diagnoses). This decline, however, may have been caused by an overall reduction in HIV testing, not a true decrease in the number of infections, leading the Department of Public Health to conclude that “drop in new diagnoses suggest that some San Franciscans with HIV may have been missed.”
“It is possible that we had fewer HIV infections in 2020. Many people stayed on PrEP, and many people also stayed at home and had less sex because of the pandemic,” said Broussard. “At the same time, I’m skeptical that there was a true decrease in HIV infections, because we saw sexually transmitted infections rebound pretty quickly after shelter-in-place. PrEP may have made the difference, but we may not know for a while.”
Reductions in HIV testing caused by COVID-19
The largest declines in HIV testing happened during San Francisco’s shelter-in-place order, which was in effect from mid-March through May 2020. HIV testing data from Zuckerberg San Francisco General Hospital, UCSF, and CPMC laboratories show reductions in HIV testing volume of 25%, 52%, and 40% in March, April, and May 2020, respectively, compared to those same months in 2019. Overall, the average number of monthly HIV tests at medical sites in 2020 was 18% lower than the average in 2019.
HIV testing at community sites like SFAF’s Magnet clinic–which likely test populations at higher risk of HIV infection–showed even bigger drop-offs during the pandemic, with an 86% reduction in the number of HIV tests completed in April 2020 compared to April 2019. Through the remaining months of 2020, monthly averages in testing were consistently 40-50% lower than in the previous year.
“We really won’t be able to see the full picture of HIV infections in San Francisco until our community HIV testing sites get back up and running at full capacity,” said Broussard. “These community clinics, which have built trusting relationships with communities most at risk for and impacted by HIV are where a lot of new infections are caught. At SFAF, we’re at about 80% of our capacity now. But many smaller sites have not been able to provide services throughout the pandemic, and that is likely having an impact on who is able to access HIV testing right now.”
New HIV diagnoses
Among the 131 people newly diagnosed with HIV in San Francisco, the largest proportion were Latinx (37%), followed by white (28%), Black or African American (21%), Asian/Pacific Islander (11%), and Native American (2%). In the past decade, the proportion of Latinx people in new HIV diagnoses has been increasing, as has the proportion of HIV cases among Black and African American community members.
Most new HIV diagnoses are men who have sex with men (61%), 4% were trans women, and 7% were heterosexual. 19% were people who inject drugs: 9% were men who have sex with men who inject drugs, and 10% were other people who inject drugs.
Women made up a higher proportion of new HIV cases last year (14%), compared to previous years (8% of new cases were among women in 2018 and 2019).
Linkage to care & HIV viral load testing
Even during the COVID-19 pandemic, linkage to HIV care and engagement in HIV care remained high for people newly diagnosed with HIV. 92% of people diagnosed in 2020 were linked to care within one month of diagnosis, and 72% remained in care for the next three to nine months. About three-quarters (77%) of people newly diagnosed achieved viral suppression within six month of their diagnosis.
Viral load testing, which is used as a measure of how engaged people are in HIV care, declined during the pandemic.
The largest decline happened in April 2020, with 52% fewer viral load tests done compared to the same month in the year previous. By March 2021, volume of viral load testing had mostly recovered to 6% below the 2019 monthly average.
PrEP
The epidemiology report estimates that PrEP coverage is high in San Francisco, with 85% of people with “an indication for PrEP” having been prescribed PrEP in 2019. Although, said Broussard, it can be misleading to assume that 85% of people in San Francisco who may benefit from PrEP have been prescribed PrEP.
“There are indicators that there are fewer individuals taking PrEP and continued disparities among high risk communities,” she said. “Toward the end of 2019, SFAF started to see decreases in the number of individuals actively taking PrEP which continued until this past April. Our PrEP navigation team has diligently tried to follow up with individuals who stop coming to the clinic for PrEP follow up appointments and support individuals experiencing barriers that want to continue on PrEP. The rate of PrEP use in persons who inject drugs in San Francisco, who may have multiple risk factors for acquiring HIV, continues to be low. We also see significant differences in PrEP access and uptake in certain parts of the Bay Area. As we rebound from the pandemic, we must work toward equity in access for communities in San Francisco and beyond.
At San Francisco City Clinic, 70% of HIV-negative clients who identify as men who have sex with men were on PrEP in 2020. Black and African American men who have sex with men were less likely to use PrEP (63%) in 2020 than white, Latinx, and Asian and Pacific Islander men who have sex with men (70% – 71%).
At San Francisco AIDS Foundation, there were 1,229 clients screened for PrEP in 2020 compared to 3,235 clients in the previous year. Broussard said that the demand for PrEP has gone up since April, 2021.
“We’re on track to exceed the number of people that we enrolled on PrEP last year,” she said. “Even before the pandemic began, we started to see our PrEP enrollments go down, due to capacity issues and some reduction in demand. But we’re rebounding, and we are on a trajectory to have about 3,000 people actively taking PrEP through our program by the end of the year.”
HIV & homelessness
As in past years, housing status played a significant role in HIV treatment and care in 2020. People without stable housing were less likely to be consistently on antiretroviral therapy, and were far less likely to maintain undetectable viral loads, which improves individual health and prevents HIV transmission.
While 95% of people experiencing homelessness newly diagnosed with HIV in 2019 were linked to care within one month, only 68% were virally suppressed a year later (88% of people with housing were virally suppressed). An estimated range of 61-86% of all people experiencing homelessness with HIV were receiving antiretroviral therapy as of December 2020, while the range for housed people was much higher (92-99%).
Correspondingly, people experiencing homelessness were more likely to experience viral loads over 200 copies/mL (i.e., they were less often “undetectable”). The report estimates that people without housing spend 44% of their time with detectable viral loads, compared to 26% for people with housing.
Read the entire report
https://www.sfdph.org/dph/files/reports/RptsHIVAIDS/AnnualReport2020-Purple_20210817Web.pdf