BREAKING NEWS: Increase in HIV diagnoses in SF from previous year; likely due to delayed testing during COVID-19 pandemic
Media inquires: media@sfaf.org; 415-487-8064
San Francisco, September 14, 2022–Yesterday, the San Francisco Department of Public Health’s Population Health Division released the HIV Epidemiology Annual Report for 2021, showing trends in the city’s HIV diagnoses and care indicators. For the first time in 9 years, there was an increase in the number of HIV diagnoses made from the previous reporting year, likely caused by testing delays during the COVID-19 pandemic. Other findings from the report highlighted continuing disparities experienced by people of color, people who use drugs, and transgender communities.
“San Francisco is a leader in HIV prevention, treatment, and care, and we have much to be proud of in our response to HIV,” said Dr. Tyler TerMeer, CEO of San Francisco AIDS Foundation. “But we know we have much more work to do in order to end the HIV epidemic. Now is not a time to pat ourselves on the back for what we’ve achieved–it’s a time for us to come together and find real solutions to end HIV transmission, care for people who use drugs, end overdose, support Black and Latinx communities, and ensure that all people living with HIV have access to testing, treatment, and care.”
Trends in HIV diagnoses
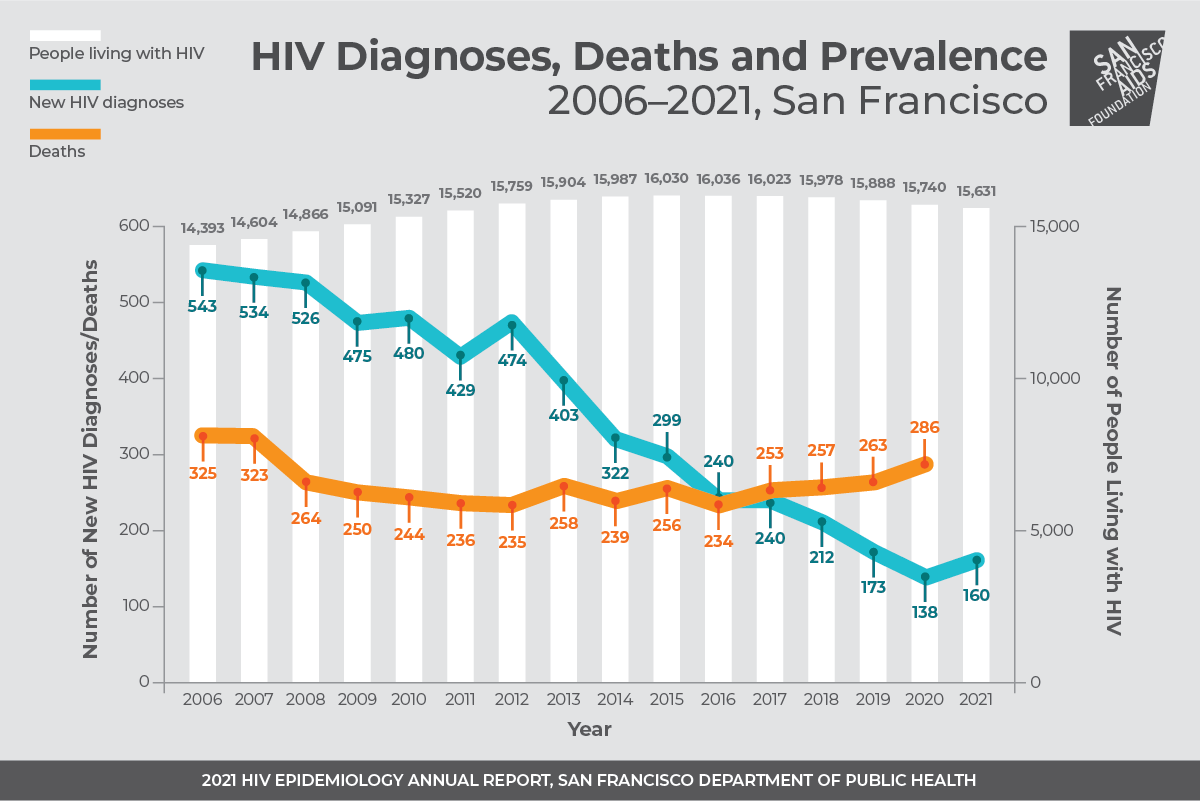
There were a total of 160 HIV diagnoses made in 2021, a 16% increase from the 138 made in 2020. This increase disrupts the decline in new HIV infections that have occurred in San Francisco year-after-year since the mid-2000s–and likely caused by disruptions to HIV testing during the 2020 COVID-19 shelter-in-place.
“[This increase] may be a result of delayed testing whereby some people infected in 2020 delayed testing until 2021,” the report says. The number of new infections in 2021 (160) is still lower than the number of new infections in 2019 (173).
The proportion of new infections among white individuals has been on the decline for many years, which means the communities of color are experiencing larger and larger shares of new diagnoses. The highest number of new infections in 2021 were among Latinx people (38%), followed by white (33%), Black/African American (16%), and Asian/Pacific Islander (9%).
A higher proportion of trans women (8%) and cisgender women (14%) were diagnosed with HIV in 2021 compared to previous years.
In terms of transmission category, there have been declines among men who have sex with men since the mid-2010s with the increased uptake of PrEP. In 2021, less than half (49%) of new HIV infections were among men who have sex with men (with an additional 14% of new infections among men who have sex with men who also inject drugs). Trans women who have sex with men accounted for 6% of infections, and people who inject drugs accounted for 27% of new HIV diagnoses.
Trends in HIV care
The percentage of people newly diagnosed with HIV who are linked to care within one month of diagnosis remains high, at 94%. Among those diagnosed in 2020, 80% were virally suppressed within a year of diagnoses. Among all people living with HIV in San Francisco, an estimated 72% were virally suppressed.
However, disparities are apparent for people without housing, people who use drugs, and people of color.
Drug overdose is now one of the leading non-HIV-related causes of death for people living with HIV, accounting for 15% of deaths from 2017-2020 (up from 10% between 2013 – 2016). This mirrors trends seen city-wide in rising rates of overdose in recent years, and reinforces the need for San Francisco to implement robust overdose prevention programs including safe consumption services.
People who inject drugs and those experiencing homelessness were far more likely to not be virally suppressed in the 12 months after their diagnoses, and experienced longer times to become virally suppressed than other populations. Only 57% of people diagnosed in 2021 (January – September) who were experiencing homelessness were virally suppressed after six months.
Between 2018 – 2020, Black and Asian/Pacific Islander individuals newly diagnosed with HIV experienced increases in the amount of time it took to achieve viral suppression (after declines in previous years), pointing to possible disruptions in care caused by the COVID-19 pandemic.
Read the full 2021 HIV Epidemiology Annual Report.









