Providing free sterile syringes is a proven way to stop the spread of HIV, hepatitis C and other infectious diseases among people who inject drugs and their sexual partners.
In addition to preventing the spread of infections, syringe access and needle exchange programs support the health and wellbeing of people who use substances in other ways, too.
- Providing access to overdose prevention resources and training
- Linking people to substance use treatment
- Facilitating safe syringe disposal
- Linking clients to housing, food resources and other social services
Frequently Asked Questions
Yes. The public health benefits to syringe access and distribution program are clear. Syringe access programs reduce new HIV and hepatitis C infections by decreasing the sharing of syringes and other injection equipment. In the U.S., the number of yearly HIV infections among people who inject drugs has been cut in half (2008 – 2014) in large part because of syringe access programs. Other research similarly supports the effectiveness of syringe access programs in reducing hepatitis C infections.
Every major medical and public health organization in the U.S. including the American Medical Association, the World Health Organization and the Centers for Disease Control and Prevention support syringe access and disposal programs. The CDC and the U.S. Department of Health and Human Services describe syringe service programs as an effective component of a comprehensive and integrated approach to HIV prevention among people who use injection drugs.
Syringe access programs are critical, lifesaving programs that prevent the spread of infectious diseases including HIV and hepatitis C. In addition to benefiting the health of people who use drugs, syringe access programs benefit communities by helping to link people to social and health services, improving public safety, reducing needlestick injuries, and preventing overdose.
Some people wonder why we provide syringes on an “as needed” basis instead of giving out only one at a time or on a return-one-to-receive-one basis. Simply put, “user-driven” models–that allow people access to as many syringes as they need–are most effective when it comes to preventing disease transmission and improving people’s lives. You can read more about the research supporting this model, here.
Unfortunately, due to the housing crisis in San Francisco, some people who use drugs are unable to safely use indoors, and some needles end up discarded improperly. That is why there are a variety of strategies used to help prevent improper syringe disposal and pick up improperly discarded syringes.
SFAF, the San Francisco Department of Public Health, our syringe access program partners, and communities of people who use drugs ensure that the vast majority of syringes that are used are safely disposed of. We ensure that this happens in a variety of ways:
- Used syringes can be returned and safely disposed at all syringe access sites across the city;
- 17 outdoor disposal kiosks are available 24/7 for folks to discard used syringes across the city; and,
- SFAF’s Pick Up Crew works 12 hours per day, 7 days per week across the city to respond in real time to improperly discarded syringes.
If you see discarded syringes, text a photo with information about the location to the Pick Up Crew at 415-810-1337. Or, you can report the syringe by calling 311.
No. Many scientific studies, including a Surgeon General’s report, show that needle exchange and access to sterile supplies does not increase drug use when conducted with referrals to both drug treatment and HIV and hepatitis C testing, medical care and support services.
Syringe access programs oftentimes facilitate referrals to drug treatment and counseling. People who injection drugs are five times as likely to enter treatment for substance use and more likely to reduce or stop injecting when they use syringe access services.
Overdose from opioids is a serious problem that claims the lives of hundreds of San Franciscans every year. Naloxone (brand name Narcan) is a medication that is safe, effective, inexpensive, and easy to administer in the case of an overdose. It is a public health tool that has been successfully used worldwide to save lives. Every year in San Francisco, thousands of people are saved from overdose because of naloxone.
People who use drugs and are ready to make a change and should have access to substance use treatment and support. Other folks may not be ready to make a change–but likewise should be supported with the health and harm reduction tools they need. Research shows that providing naloxone doesn’t encourage people who use opiates to increase their drug consumption, and it doesn’t increase the likelihood that they will harm themselves or other people around them.
If you see syringes on the street, do not touch or try to move them. If you live in San Francisco, text a photo and location of the syringes to the San Francisco AIDS Foundation Pick Up Crew at 415-818-7769.
You can also report discarded injection equipment to 311.
There are many benefits of syringe access programs to both people who use drugs and the community. In addition to improving the health of people who use drugs, syringe access programs prevent overdose and save lives, reduce accidental needlesticks by facilitating safe disposal and facilitate referrals to other mental health and social services.
Syringe access programs also improve public safety and safer syringe disposal by providing people with safe options for disposal.
In the U.S., federal funds may now be used to support the syringe access programs in order to prevent new HIV and viral hepatitis infections in communities with a demonstrated need. Although federal funding may be used to support many services at syringe access programs, at this time federal funding may not be used to purchase sterile needles or syringes.
Accidental drug overdose is the leading cause of death in the U.S. for people under age 50. Nearly two-thirds of overdose deaths in 2016 were caused by a prescription or illicit opioid.
The Drug Policy Alliance identifies many complicated reasons attributed to the current opioid and overdose epidemic. This includes but is not limited to the over-prescription of opioids, stigma associated with drugs use, lack of access to overdose prevention education and resources and fentanyl entering the drug supply.
There isn’t a simple solution to end the opioid and overdose epidemic, but there are things you can do to educate your community and help prevent overdose deaths. Learn more from the Drug Policy Alliance about how to recognize and respond to an overdose, support effective harm reduction and treatment strategies and get involved in advocating for the health of people who use drugs.

What Is Harm Reduction?
We respect the rights and dignity of people who use drugs. Syringe access programs are based in harm reduction, a philosophy that seeks to reduce the harms associated with drugs and alcohol without judgement. Harm reduction is a way to “meet people where they’re at,” without requiring you to meet certain conditions in order to maintain your health. It’s safety, your way.
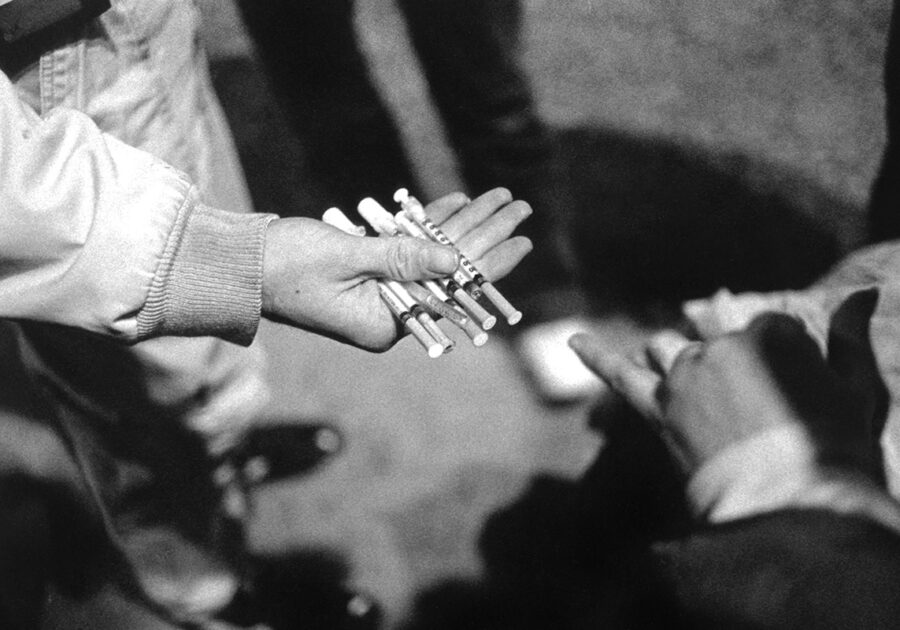
User-Driven vs. Needle Exchange
Needle exchange and syringe access programs are proven to reduce disease transmission and connect people to treatment and other medical services. These programs benefit public health. Comparing models for syringe access shows that user-driven access, those programs where the participant defines how many syringes they can receive, benefits health the more than one-for-one or one-for-many exchange models.
See Improperly Discarded Syringes?
Help us keep San Francisco neighborhoods safe and clean. Notify our Syringe Pickup Crew. We’ll come by to safely dispose of the discarded syringes.
Send a text message to 415-818-7769 (send a picture and the location)





